Mental health is critical to overall well-being, and access to quality mental health care is vital for individuals of all ages. The National Institute of Mental Health estimates that 22% of American adults experience a mental illness at some point each year. According to the Centers for Disease Control and Prevention, people 65 and older have an increased chance of developing mental health problems like sadness and anxiety.
As the primary health insurance program for Americans aged 65 and older, Medicare plays a significant role in providing access to essential healthcare services. However, understanding the scope of Medicare’s coverage for mental health services is vital.
This comprehensive guide seeks to clarify the possibilities and restrictions for mental health care coverage under Medicare.
Understanding Medicare

It consists of different parts, each serving specific purposes. Medicare Part A offers hospital insurance, Part B provides medical insurance, Part C encompasses Medicare Advantage plans, and Part D focuses on prescription drug coverage.
Eligibility for Medicare is primarily based on age, but individuals with certain disabilities may also qualify. Understanding the different parts and eligibility criteria is crucial to navigating and maximizing the Medicare program’s benefits.
Medicare Part A and Mental Health Coverage
It also known as hospital insurance, offers coverage for mental health services provided on an inpatient basis; this includes mental health care received during a hospital stay, such as psychiatric evaluations, counseling, and necessary medications. However, it’s important to note that Part A has limitations and restrictions.
A qualifying hospital stay is typically an eligibility requirement for coverage, meaning the individual must meet specific length and type of stay criteria. Understanding these coverage details is essential for individuals seeking mental health care under Medicare Part A.
Medicare Part B and Mental Health Coverage
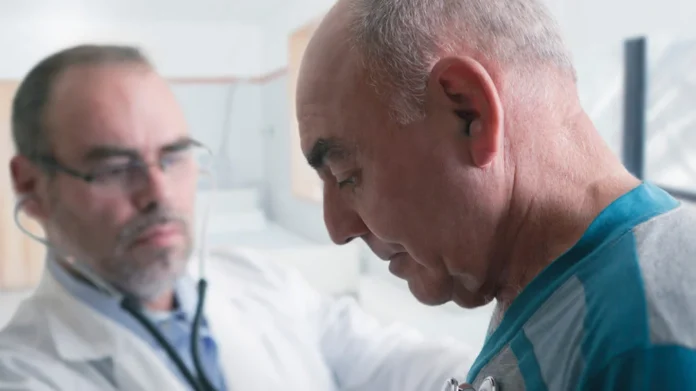
Mental health services are mostly covered under Medicare Part B, a crucial element of the Medicare program. Counseling, therapy sessions, psychiatric assessments, and medication administration are just a few of the outpatient mental health care treatments that Part B extends its coverage. These programs are crucial for people looking for assistance and therapy outside of a hospital setting.
People need to be aware of the scope of the Medicare Part B coverage they are eligible for to obtain the appropriate outpatient mental health care necessary to address their mental health effectively.
Mental Health Coverage under Medicare Advantage (Part C)
In contrast to Original Medicare (Part A and Part B), Medicare Advantage (Part C) plans offer a different method of getting Medicare benefits. These Medicare-approved private insurance plans incorporate Parts A and B coverage while frequently providing extra benefits. Private insurance providers offer them. Mental health coverage under Medicare Advantage includes essential services such as counseling, therapy sessions, and psychiatric evaluations.
Certain Part C plans may even extend coverage to encompass expanded mental health services or prescription drug benefits, ensuring comprehensive care beyond the scope of Original Medicare. Familiarizing oneself with these options facilitates selecting a plan that effectively addresses individual mental health needs.
Prescription Drug Coverage (Part D) and Mental Health Medications

Comprehensive prescription drug coverage holds significant importance for individuals managing mental health conditions. Medicare Part D is crucial in ensuring coverage for mental health medications. You can learn more about Medicare part d by visiting this page. It guarantees access to various drugs to treat mental health disorders, encompassing antidepressants, antipsychotics, and anti-anxiety medications. Part D plans comprise various coverage tiers, with differing levels of cost-sharing contingent upon the specific medications.
Individuals can efficiently manage their prescription demands for mental health while maximizing their healthcare budget through an awareness of the coverage options and related costs within Medicare Part D.
Limitations, Exclusions, and Coverage Restrictions
Though extensive, Medicare’s mental health coverage entails certain limitations and exclusions that individuals should understand. Coverage restrictions may exist for specific types of therapy, treatments, or providers. For instance, it may limit the number of covered therapy sessions or restrict coverage to evidence-based treatments.
Additionally, certain services may necessitate prior authorization or adherence to specific requirements to qualify for coverage. Having a clear understanding of these limitations and coverage restrictions empowers individuals to navigate their mental health care effectively within the parameters of Medicare and avoid unexpected expenses.
Medicare Mental Health Resources and Additional Support

Medicare recognizes the importance of comprehensive mental health care and offers beneficiaries a range of resources and support. Preventive services such as screenings and counseling are available to promote early detection and intervention.
Moreover, support networks, helplines, and community organizations exist to aid individuals in accessing mental health services. Leveraging these Medicare-provided resources can significantly enhance the overall mental well-being of beneficiaries. By tapping into these additional avenues of support, individuals can find the necessary assistance to address their mental health needs effectively.
Does Medicare Provide Coverage for Every Mental Health Condition?
Although it offers coverage for a broad range of mental health services, it does not provide coverage for all mental health conditions. For instance, counseling or therapy for marital or relationship issues is not covered by Medicare.
Furthermore, Medicare does not cover services associated with developmental disorders like autism or treatment for substance abuse disorders. Nevertheless, certain state programs or Medicaid might offer coverage for some of these services.
Conclusion
In conclusion, having a comprehensive understanding of Medicare’s mental health coverage options is vital for individuals seeking holistic healthcare. The many Medicare components, including Part A, Part B, Part C, and Part D, and their specific coverage for mental health services, have been covered. It is essential to be aware of any restrictions on coverage, exclusions, or limitations that may be in place to guarantee sufficient access to mental health care.
Additionally, we have emphasized the importance of utilizing available mental health resources and support networks provided by Medicare. As you navigate your individual coverage needs, seeking professional advice can further assist in making informed decisions.
Remember to prioritize your mental health and seek the necessary care and support under Medicare.