A car crash can leave you shaken even if the damage looks minor. In the hours after, adrenaline can mask pain, and you might tell yourself you are fine.
Then the stiffness hits later. Or headaches start the next day. Or you notice you cannot turn your neck without wincing. This is where seeing a car accident doctor matters.
The goal is not to be dramatic. It is to get properly evaluated, document what is going on, and start care early so small problems do not become long term ones.
This guide explains what a car accident doctor does, when to go, what to expect at your visit, and how follow up care usually works.
It is written to help you make calm, practical decisions when you are dealing with a stressful situation.
When should you see a car accident doctor after a crash?

You should see a medical professional as soon as possible after any crash that causes pain, symptoms, or a significant jolt to your body.
Even if you feel mostly okay, an evaluation can catch injuries that are easy to miss at first. Early care also creates a clear medical record that ties symptoms to the accident, which can matter later if issues worsen.
What symptoms mean you should get checked right away?
Certain symptoms are a clear signal to seek medical care immediately, especially if they are new after the collision.
Persistent headaches, neck pain or stiffness, and back pain that limits movement should be evaluated sooner rather than later.
Dizziness, nausea, or a foggy feeling can point to concussion type symptoms and deserve prompt attention.
Numbness, tingling, or weakness in your arms or legs should not be ignored because these can suggest nerve involvement.
Chest pain, shortness of breath, or abdominal pain can indicate more serious issues and should be treated as urgent.
Noticeable swelling, bruising, or joint pain may also require assessment to rule out structural injury. If pain interferes with sleep, or if anxiety and panic symptoms feel overwhelming, it is still valid to get checked.
If you have severe symptoms, signs of concussion, or any concern about internal injury, emergency care is the safest choice.
Why do injuries show up later?
After a crash, adrenaline and shock can temporarily dull pain signals. Inflammation also takes time to build. That is why people often feel worse 24 to 72 hours later.
Soft tissue injuries, mild concussions, and back strain are classic examples. Waiting too long can mean you push through pain, move differently to compensate, and irritate the injury further.
What does a car accident doctor do that is different from a regular visit?

A car accident visit is still medical care, but it is more focused on identifying accident related injuries and planning recovery.
A car accident doctor typically looks at your symptoms in the context of impact forces, your position in the vehicle, seat belt involvement, and what parts of your body absorbed the force.
What information will the doctor ask for?
Expect the doctor to ask when the crash happened and when symptoms began, because the timeline matters.
They will likely ask where you were sitting, whether you wore a seat belt, and what kind of collision occurred, such as a rear end impact or a side impact.
Airbag deployment can change the type of injuries they look for, so that often comes up too. They may ask if your head hit anything or if you lost consciousness, since those details affect concussion screening.
You will also be asked what hurts now, what movements make symptoms worse, and whether you have had similar pain or injuries in the past.
These answers help the doctor decide what to examine closely and whether imaging or referral is needed.
How does the exam usually work?
Most visits begin with vital signs and a brief medical review, then move into a focused exam of the painful areas. The doctor will often check range of motion in the neck, shoulders, back, hips, and knees, depending on your symptoms.
Neurological screening is common and may include checking sensation, strength, reflexes, and coordination, especially if you report tingling or weakness.
They may press on specific muscles and joints to locate tenderness and spasm, and they may do balance or cognitive checks if concussion is suspected.
The goal is to identify both obvious injuries and subtle red flags.
Which injuries are most common after car accidents?

Not all crashes cause the same injuries, but there are patterns that show up often.
What is whiplash and how is it treated?
Whiplash is a neck injury caused by a rapid back and forth motion, most common in rear end collisions.
Symptoms can include neck pain, stiffness, headaches, shoulder pain, and reduced mobility.
Treatment often focuses on short term symptom relief paired with safe movement so the neck does not stiffen further.
Many care plans include gentle stretching, posture guidance, and a gradual return to normal activity.
Physical therapy or guided rehab exercises are also common, especially when pain persists or range of motion is limited.
The best plans tend to focus on safe movement and gradual strengthening rather than long term immobilization.
What about back injuries and sciatica?
A crash can strain muscles, irritate joints, or aggravate discs in the spine.
Lower back pain may feel like deep soreness, sharp pain with movement, or nerve like pain that travels down the leg.
A doctor may recommend a structured rehab plan to restore motion and strength while monitoring for signs that suggest nerve irritation.
Imaging may be considered if pain is severe, if symptoms persist, or if there are neurological issues like numbness or weakness.
If the symptom pattern suggests disc involvement or another condition that needs specialized care, referral to an appropriate specialist may be recommended.
Some people also need temporary work restrictions or activity modification while healing.
Can you have a concussion without hitting your head?
Yes. The brain can move inside the skull from the force of a sudden stop, even without a direct head impact.
Common symptoms include headache, dizziness, nausea, sensitivity to light, confusion, and feeling slowed down.
Concussion care usually starts with a careful symptom review and a neurological screening, then shifts into recovery guidance that balances rest with gradual, light activity.
Follow up matters because symptoms can evolve over days, and you want clear instructions on what is normal, what should improve, and what warrants urgent evaluation.
If symptoms worsen, or if there is repeated vomiting, severe headache, increasing confusion, or fainting, urgent evaluation is important.
Are soft tissue injuries “minor”?
Soft tissue injuries affect muscles, ligaments, and tendons. They are common and can be painful.
They are sometimes called “minor” because they do not show up on X rays, but they can still disrupt daily life and take time to heal.
These injuries often respond best to a thoughtful plan that combines pacing, movement, and progressive strengthening rather than complete rest.
What tests or imaging might be needed?
Not everyone needs imaging, but the doctor may order tests if symptoms suggest a more serious injury.
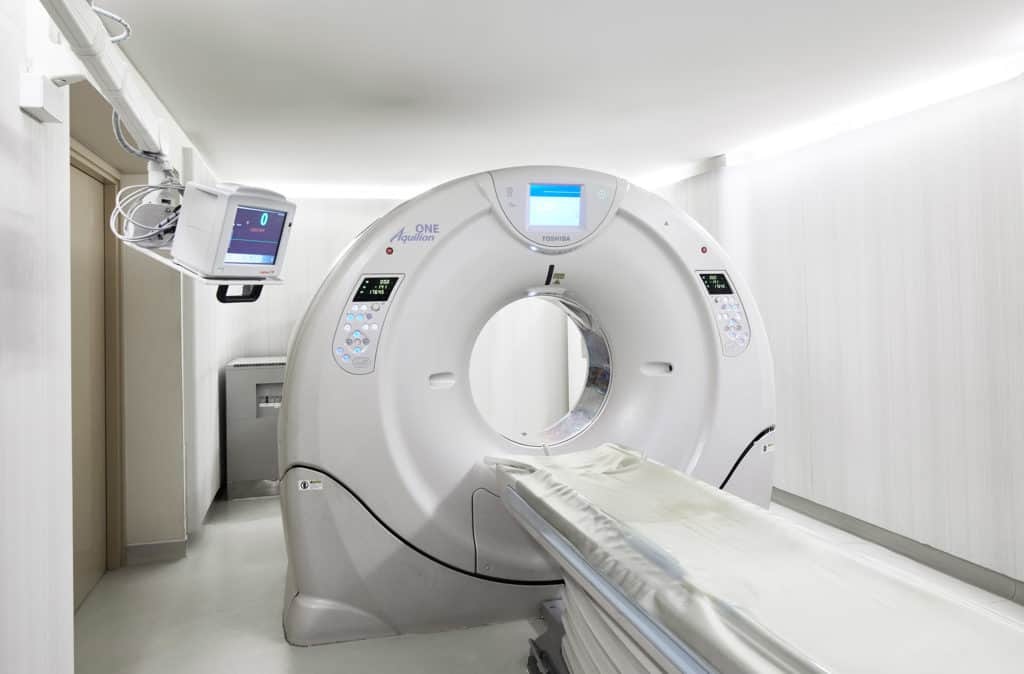
When are X rays, CT scans, or MRI used?
X rays are commonly used to rule out fractures or major alignment issues, particularly after higher impact crashes or when pain is localized and severe.
CT scans are often used in emergency settings, especially when there is concern about head injury or complex trauma that needs fast imaging.
MRI is typically used when soft tissue injuries are suspected, or when symptoms suggest disc issues or nerve involvement, particularly if symptoms persist beyond the early recovery phase.
The decision is usually based on symptom severity, neurological findings, and the mechanism of the crash.
What about “no findings” on imaging?
It is common for imaging to look normal even when someone is in pain, especially with soft tissue injuries. That does not mean symptoms are imaginary.
It often means the issue is muscle strain, ligament irritation, or inflammation that imaging does not capture well.
A clear treatment plan can still make a big difference, even without a visible finding on scans.
How does treatment and recovery usually work?

Recovery is often a combination of symptom relief, restoring mobility, and rebuilding strength. The specific plan depends on your injuries and your baseline health.
What does a typical care plan include?
Many plans include pain and inflammation management combined with guided stretching and mobility work.
Physical therapy or rehab sessions are often used to rebuild strength, improve posture, and help you move normally again.
Most people also get a simple home exercise routine and pacing guidance so they do not overdo it on good days.
Follow up visits matter because the plan should evolve as pain decreases and function improves.
If symptoms do not follow a normal recovery pattern, the doctor may recommend referrals to a specialist for additional evaluation.
How long does recovery take?
Some people feel much better in a few days. Others need weeks to months, especially with back injuries or concussion symptoms.
Recovery timelines vary based on crash severity, the type of injury, how quickly care started, and whether you can rest and avoid reinjury.
Stress levels, sleep quality, workload, and pre existing conditions can also affect how fast you improve. The most important part is monitoring progress.
If symptoms plateau or worsen, it is a signal to re evaluate.
Why is documentation important after an accident?
Medical documentation creates a clear timeline of symptoms, exams, diagnoses, and treatment. This matters for your own care because it helps track what is improving and what is not.
What should you keep track of?
Even simple notes can help, especially during the first couple of weeks. It is useful to write down when symptoms started, how they change day to day, and what triggers pain.
Tracking sleep quality, headaches, and any numbness or tingling can also give your doctor a clearer picture.
If you try medications, note what you took and whether it helped. It can also be useful to record how symptoms affect work, driving, or daily tasks.
Bring these notes to follow ups so your provider can adjust treatment based on real patterns.
What if you delay care?
Delays can make it harder to connect symptoms to the crash, especially if you return to normal activity and aggravate things. Even if you feel okay, a checkup can give you clarity and a baseline.
How do you choose the right car accident doctor?
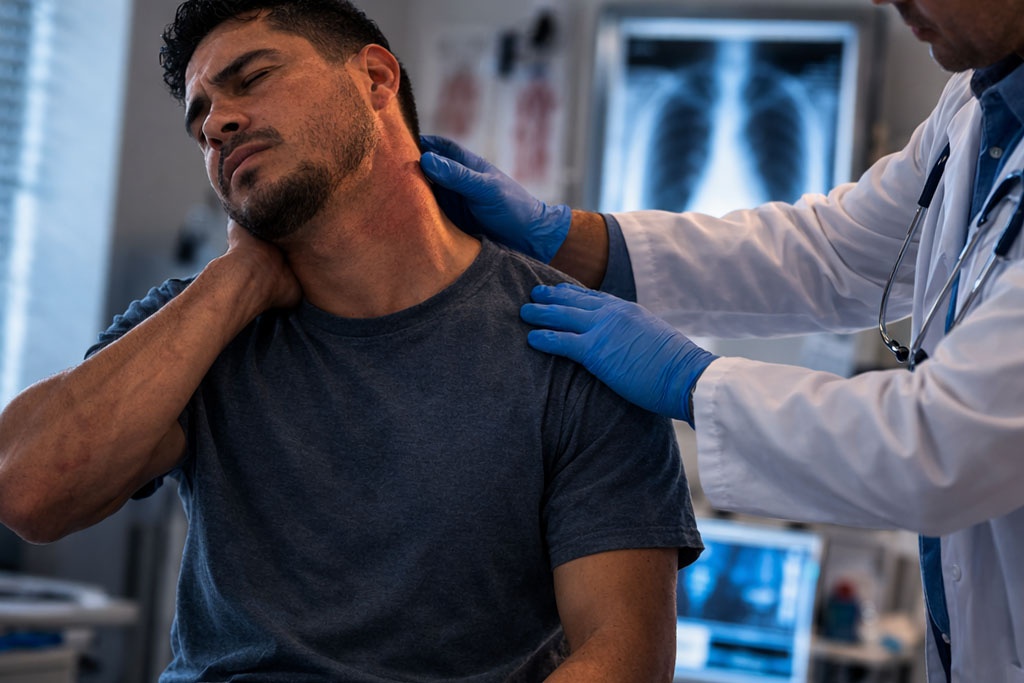
Not every provider approaches crash related injuries the same way. A good fit is someone who listens closely, explains clearly, and gives you a structured plan, including when to escalate care.
What should you look for?
Look for someone with experience evaluating accident related injuries and a communication style that makes you feel understood.
A good provider should explain what they think is happening and what the plan is, without being vague or dismissive.
It also helps when they are willing to refer you out if needed, since some symptoms call for specialty care.
Ideally, the treatment approach includes rehab or physical therapy when appropriate, and follow up is consistent so your progress is tracked.
If you feel rushed, dismissed, or pressured into a one size fits all plan, it is reasonable to seek another opinion.
Should you start with urgent care, ER, or primary care?
The best starting point depends on your symptoms. Emergency care is appropriate for severe pain, neurological symptoms, head injury concerns, chest pain, breathing trouble, or suspected fractures.
Urgent care can be a good option for moderate symptoms that need quick evaluation when the ER is not necessary.
Primary care can work well for mild symptoms or follow up care, especially if you can be seen quickly.
Some people also choose an accident focused clinic for ongoing musculoskeletal symptoms because these clinics often have structured rehab options. If you are unsure, err on the side of being evaluated sooner.
What can you do at home while you wait to be seen?

Home care should be gentle and safe. If symptoms are severe, get medical care first.
Practical steps that often help
Rest is helpful, but complete immobility can make stiffness worse, so light movement as tolerated is usually a better balance. Hydration and sleep support healing, so it is worth treating those as part of recovery, not a bonus.
Avoid heavy lifting, intense workouts, or activities that spike pain, especially in the first few days.
Many people use ice or heat depending on what feels best, and it can help to limit screen time if you have concussion like symptoms such as headaches or light sensitivity.
If you develop worsening headaches, increasing dizziness, weakness, numbness, confusion, or significant new pain, seek urgent care.
What should you take away from this?
A crash can cause injuries that are not obvious right away. Seeing a car accident doctor early helps you understand what is happening, start a recovery plan, and avoid letting manageable injuries linger.
The process is usually straightforward: a focused exam, a clear plan, and follow-up care that adjusts as you improve.







